 The more we can do to treat patients in the home helps with both utilization and the cost of care.ģ. If fewer individuals are going to the ER, then there isn't a need to bring on more staff to treat them at the ER. This reduction in utilization not only lessens the system burden by freeing up beds in the ER but also affects costs. Now that organizations are considering more proactive methods to administering care to patients beyond the four walls of the hospital, proven technologies can play a key role in making these goals attainable.Īs more payers seek to reduce unnecessary utilization, they can explore PERS and RPM technologies that offer more time-sensitive treatment and reduce the inclination for patients to go to the emergency room (ER) for care. If we can reduce the burden on these staffers while also making the patient experience more meaningful, we can generate user satisfaction and retain our tireless workers.Ĭonnected care technology is a critical component of the utilization and cost dynamic in healthcare. The work that clinical frontline staffers are trying to do is important, but they also have more on their plate than ever. A recent survey conducted by Morning Consultfound that since February 2020, 30% of healthcare workers have either lost their jobs or quit. Utilizing technological features that are easy for senior adult patients to use and provides them with a sense of comfort while receiving consistent care goes a long way towards satisfaction and engagement.Īdditionally, since we're amid a healthcare worker shortage that is only getting worse these tools can help mitigate the labor gap. 
Payers can benefit from tools or processes that boost the patient experience, especially as more quality standards account for this metric. "Information on how the innovation incorporates into provider workflow, the ease of use for patients/consumers and impact on quality of life (not just improved health) must become routine parts of clinical evidence development."īelow are five ways these new technologies and care delivery models can assist health insurers to achieve the quadruple aim. "All stakeholders need to collaborate to document and develop evidence on connected care innovations aligned with the Quadruple Aim," the blog post read. Similarly, a HIMSS blog post published in June recommended the adoption of connected care solutions, such as personal emergency response systems (PERS) or remote patient monitoring (RPM), to support efforts to accomplish the Quadruple Aim.  
"Leveraging simulation and human factors will support a resilient and sustainable response to the pandemic in a transformed health care landscape," the researchers wrote. The study underscored how new technologies and human factors can boost the patient experience, promote population health, drive down costs, and improve health worker wellness. 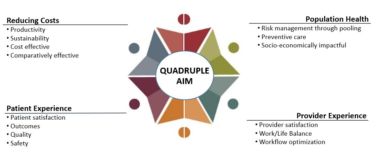
Research recently published in the American Journal of Medical Quality detailed the pursuit of the Quadruple Aim throughout the COVID-19 pandemic and the subsequent opportunities to reshape the traditional healthcare delivery model. While it's a noble ambition to focus on enhancing the patient experience, improving population health, reducing costs, and improving the work life of healthcare providers, it takes a lot of effort to make that happen.Īs with any industry-related goal, the Quadruple Aim can be best achieved through targeted investments of resources and innovations. For health insurance executives, pursuing the Quadruple Aim is the name of the game. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
